A MULTI-million pound injection has transformed the busiest accident and emergency department in Greater Manchester.
The Royal Bolton Hospital has not only redesigned its casualty department to provide a modern department — but is also changing the way it works to ensure patients get the best possible care from the start.
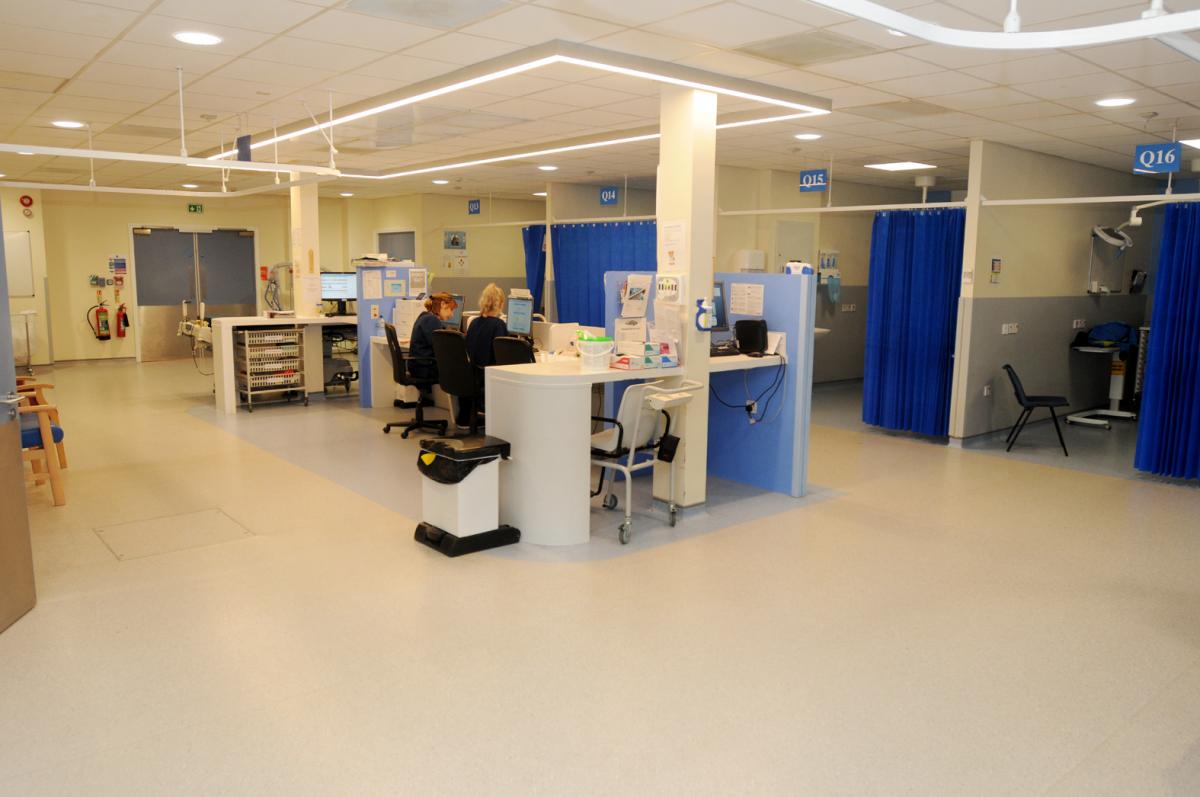
Gone is the chaotic image of patients waiting on trolleys to be replaced by a calmer and more efficiently run department, with more bays and state-of-the-art equipment.
The transformation began in 2017, with a new extension, more treatment bays - and say health chiefs the work has improved the staff and patient experience.
Andy Ennis, Bolton NHS Foundation Trust Chief Operating Office, said: "Manchester Royal Infirmary for instance gets around 240 attendances, Salford around the same and we get about 320 a day on average.
"So attendance wise we were often overwhelmed simply because our design was not big enough.
"We started about three years ago investing in improving the site, of course it is limited because we didn't build a new A&E we had to work with the spaces and the place we had."
The work was done in stages, creating the new environment and now work will concentrate on improving the way the department operates.
Accident and Emergency is made up of three areas — majors, minors and paediatrics. Health planners were commissioned to redesign the environment.
"We asked what should we have for the population we have. Their answer we should have six resuscitation bays for adults and 21 major spaces.
"We had 12 majors and four resuscitation bays," said Mr Ennis.
The difference between the old and the new is sharply brought into focus with just five bays (treatment beds)in the new extension, compared to 12 in the same size space in the original building.
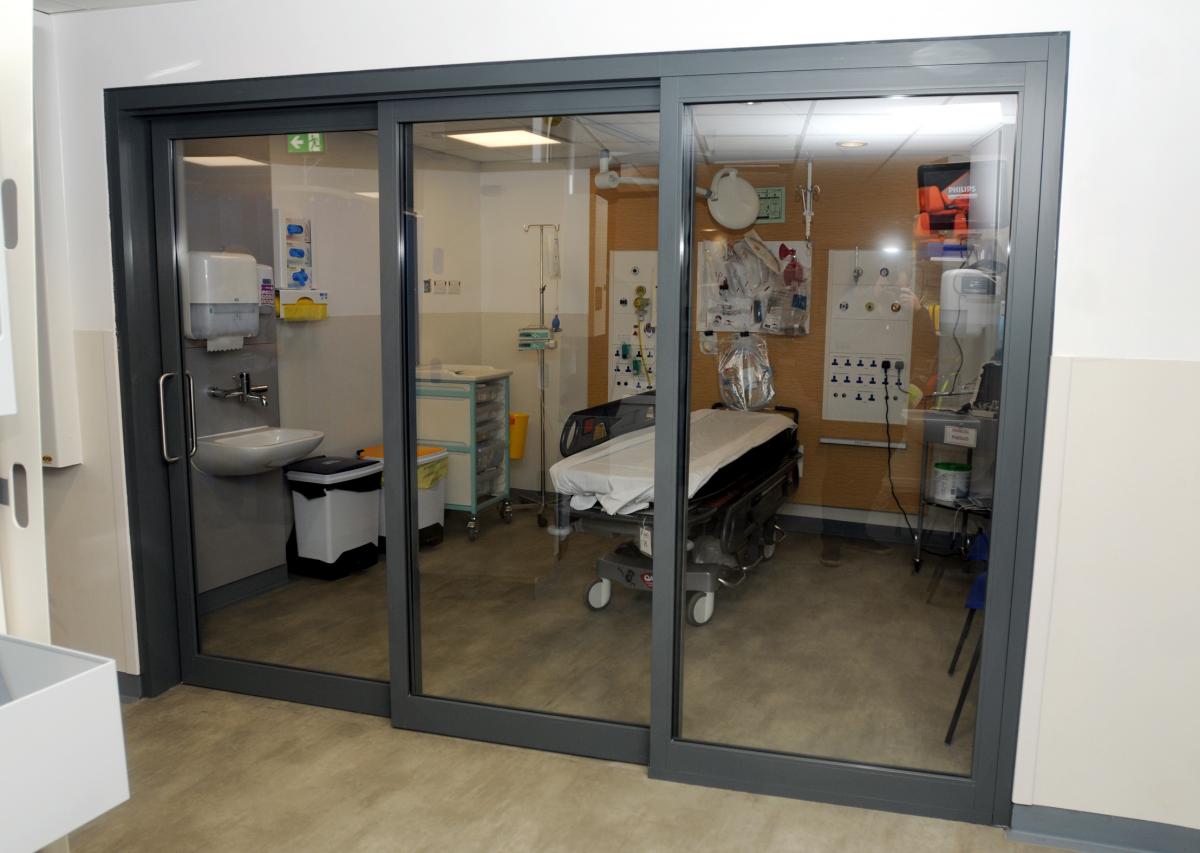
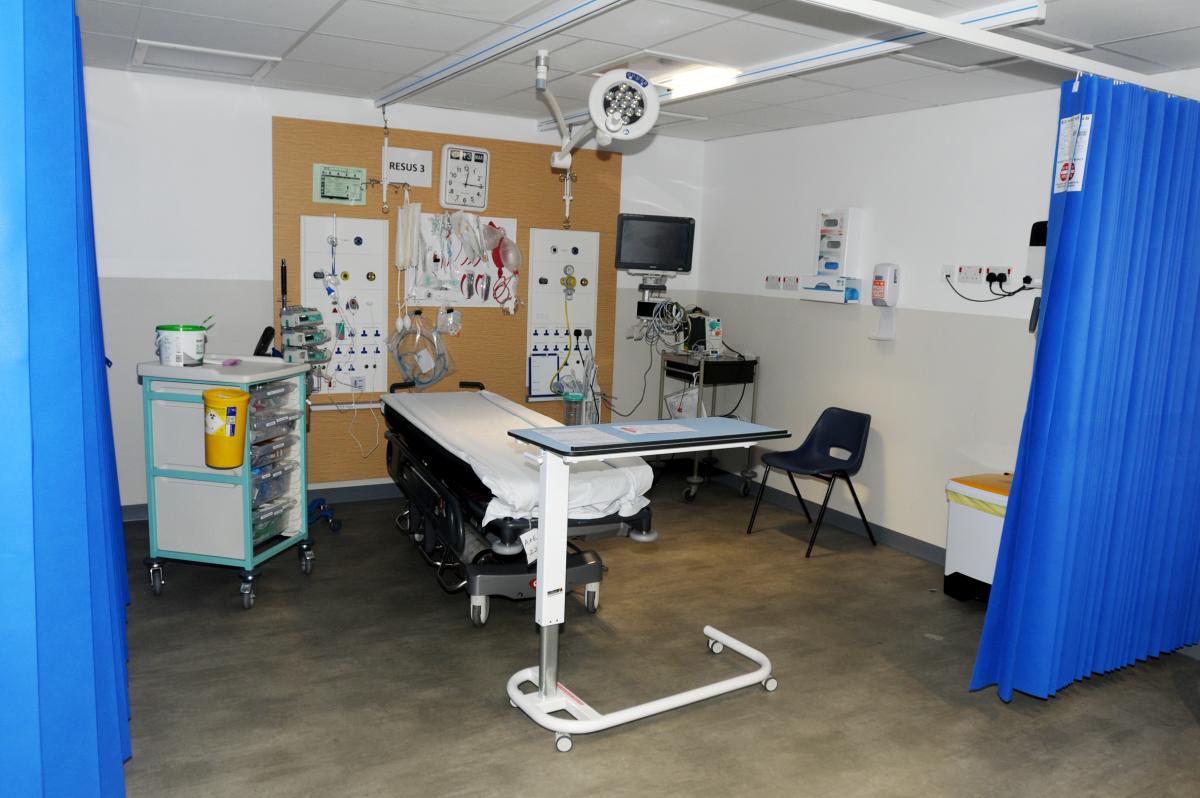
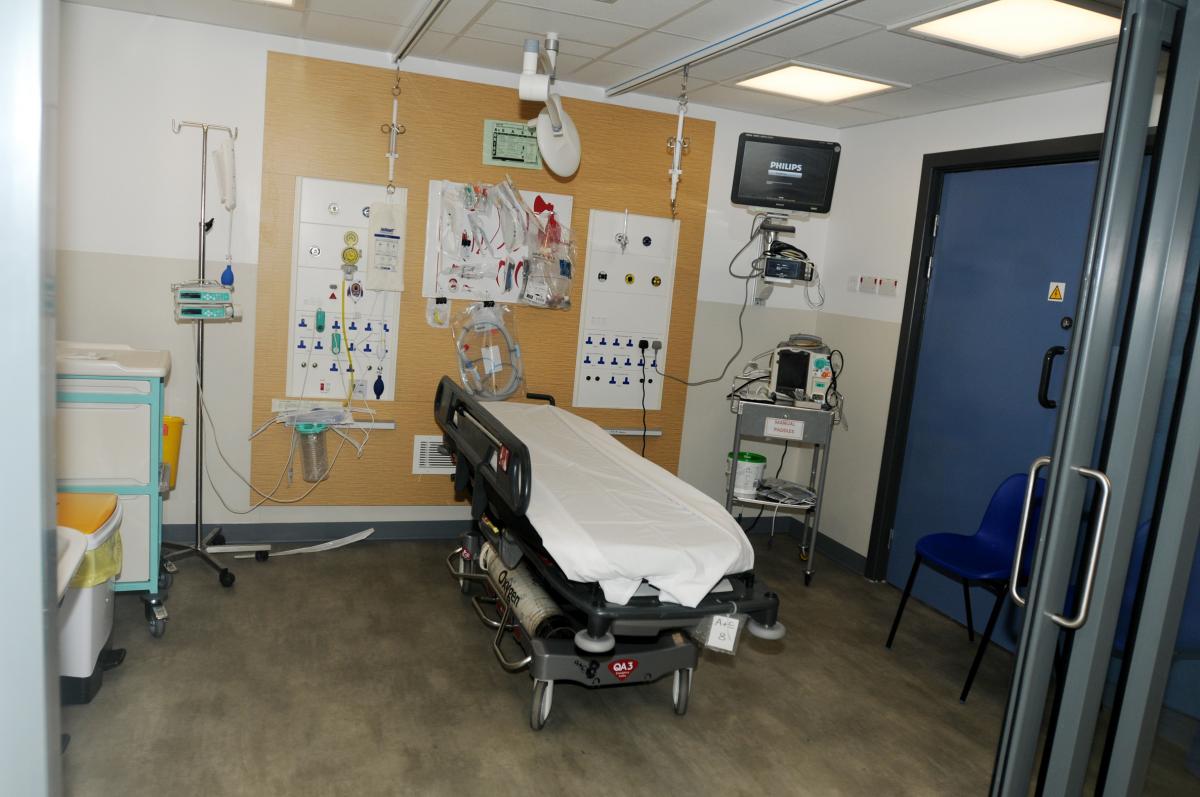
Highlights include the creation of a new modern resuscitation area — which includes two bays with glass doors — in what was an old office bloc.
The old resuscitation area is now an ambulance drop-off bay, which frees up paramedics more quickly.
"We have done a lot of work to improve our A&E performance and it is getting better, but the environment was such when we got volume in the evenings we often got that horrible picture, which papers love, of trolleys all around. Even if we were well performing sometimes when you had that surge of patients you were going to end up with that situation of trolleys around the nurses' station — it was just not a good experience for patients or staff, and we don't get that anymore," said Mr Ennis, "The resuscitation space is so much better. We needed six spaces and they needed to be better.
"There were four spaces with a curtain between and that was it, and the space was just about the space of an ambulance trolley and somebody else standing by it.
"Staff were beaming when they went into the new space. Two of the rooms have got glass doors, and now when we get someone who we know is an infection risk we can put them there and we can see them and they are safe and we are safe.
"They are now about twice the size and there is a nurses station in the middle and they can see the patients around, it's a better environment.
"The nurses station was a line of cupboards and a table top — there wasn't a nurses or doctors's station."
The hospital also has a new minor injuries unit,with its own waiting room and own team to deal with people who have not suffered a major trauma.
A new kitchen has been created for relatives and friends of patients to use.
TRANSFORMING THE WAY A&E OPERATES

Now, health bosses are focusing on changing the way the department works to ensure patients are not waiting around in a ward for a day or more to be referred to the right medics.
A new streaming system will be in place and new elderly frailty assessment area created.
Mr Ennis explained: "The current model of our A&E you are filtered out when you arrive and we are changing that. We are going to have a system at the front where we will assess you first, clearly if you come in with a major incident — having as a heart attack — then you are going straight into resus, that doesn't change.
"But we want to create an environment which says you don't need to go A&E we need to get you see by a another practitioner, we are going to stream you to over there.
"The four hour window, can cause problems because everybody irrespective has to be treated within four hours, it is a good target, but is very blunt and rushing an elderly patient to meet the target is often the wrong thing to do
"We want to create that area where patients can be assessed."
"What we are trying to do in streaming is a bit different to everyone, we are being a pushing that boundary a bit more and expanding it — in the long term about 1/3 of patients who come to A&E could probably be streamed away.
"The aim is we do the assessment at the front door, and we might decide that they need to come in but the great news is we have done the diagnosis ,we have started the first treatment and know exactly what we are doing, rather than doing a quick assessment in A&E and send them to a ward.
"And during the ward round the next day and the assessment takes place and suddenly the patient is in for 24 or 48 hours before they have even been assessed —we are going to put the assessment right at the front door and make sure you get the right treatment at the start."
"Now we created the space to put that in place in time for next winter."
I










Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereLast Updated:
Report this comment Cancel